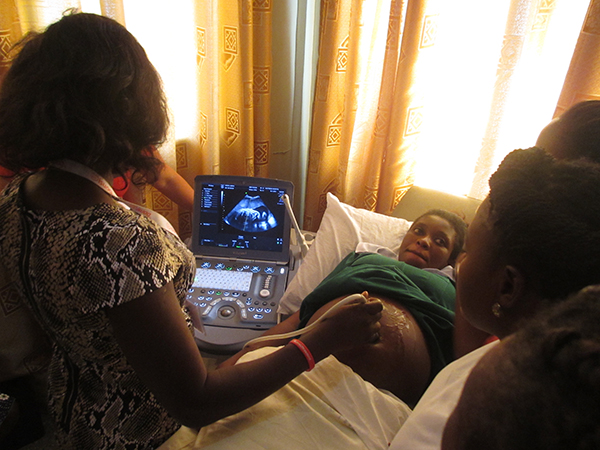
Client Satisfaction Soars from a Positive Intervention
Cervical cancer is a malignant tumor of the cervix affecting the lower part of the uterus and it is one of the leading causes of death in women. It occurs mostly in women over 30 years. It is a condition that can have no symptoms though some may experience pain in the pelvis, pain during sex, bleeding after sexual intercourse and abnormal bleeding from the vagina.
Management of this condition includes chemotherapy, cryotherapy, surgery such as hysterectomy, cervicectomy and others depending on the stage of the disease.
Over the past three years, 3456 women in the reproductive age in 70 communities spread over seven districts of the Ashanti region were screened by Women’s Health to Health through the mobile clinic program to detect early abnormalities that can lead to cancer of the cervix. The women are screened for this condition by visual inspection of the cervix by applying 5% Acetic Acid (VIA) on the cervix and inspecting for signs of pre-cancerous cells. Women found to be VIA positive were referred to Kumasi South Hospital and Komfo Anokye Teaching Hospital for management.
To alleviate the struggle and stress that these women to go through when referred to these facilities for cryotherapy, Women’s Health to Wealth has purchased a Cryotherapy machine to manage women who are VIA positive and require cryotherapy in an efficient stress free manner at an affordable cost. . This service is not limited to referrals from WHW mobile clinics but also to many women who require cryotherapy referred from other from other public facilities.
Indeed, this is has come as a great help to women who previously had to wait out an average of 4 to 6 months to be scheduled for cryotherapy at the Kumasi South Regional Hospital that was the main and cheapest source for this treatment. Clients can now have the treatment provided at suitable cost within 10 days after the diagnosis. The staff of Women’s Health to Wealth and especially clients are thankful to the management for this initiative as it has yielded very positive results in terms of client and job satisfaction.
Story By
Beatrice Nyamekye (Health Coordinator).
Greater Works Restoration Foundation (GWRF) recently held a free surgical outreach to the Upper East Region.
The programme was extremely successful and the impact was significant in the lives of the individuals we operated on.
Thirty (30) successful free reconstructive surgeries were performed. Eighty five( 85%) percent of the patients seen were women and children with all forms of anomalies ranging from birth defects to acquired traumatic events of which post burns deformities were common.
Below is a summary of how the items donated were used.
- The little teddy bears were given to the children to calm them down before and after the surgeries
- The pain medication was given to children post-operatively to control pain
- We donated some boxes of examination gloves and a box of drugs (Advil) to the administration of the regional hospital.
- On our last day, we made a very long drive to SIRIGU, on challenging terrain to an orphanage for babies and toddlers where we donated some of the blankets and teddy bears you gave us.
[PHOTOS] Training with ISUOG
Dehydration in children younger than five years of age as a result of diarrhea and vomiting, malarial fever and other infections, is a major contributory cause of mortality in under-5s in Ghana. The ominous nature of dehydration in children warrants an immediate and effective restoration of body water balance, to forestall death. Reducing child mortality has been a key goal of the international community for decades; improving child and family health, perhaps the most essential goal for women worldwide, is a critical objective of Women’s Health to Wealth and WomenStrong International.
The Komfo Anokye Teaching Hospital (KATH) Pediatric Emergency Unit, or PEU, is where children with such acute febrile conditions as severe malaria, diarrhea, vomiting, bacterial and viral infections and other acute medical conditions are initially admitted and stabilized before being transferred to wards for further treatment or discharged.
Severe diarrhea and vomiting, either as an additional symptom to an underlying disease or as a diagnosis itself, is the third most frequent cause of admission to the PEU. In July 2015, Women’s Health to Wealth donated 30 cases of DripDrop® Hydration Powder to the PEU, containing 5760 units of 10g packs, to assist the unit in the effective management of dehydration of children with indicative conditions.
The most widely used cure for rehydration, for these diseases as for severe malnutrition, is oral rehydration solution, or ORS, which combine sugars, salts and other ingredients and which is credited with saving some three million children annually. Most of the solutions on the market don’t taste very good, however, meaning that children well enough to balk at the unappetizing or medicinal taste simply won’t drink the stuff. The formula for DripDrop®, developed by a San Francisco-based family physician, Dr. Eduardo Dolhun, combines medical-standard hydration with child-friendly flavors, making it easier and more appealing for children to get the solution down and to finish the course of treatment. Dr. Dolhun’s ORS product has gained wide acceptance in hospitals and is now marketed through his own firm, DripDrop Inc.
In September, two months after the DripDrop donation was made, WHW paid a follow-up visit to KATH’s PEU to discuss with the staff the usefulness or otherwise of the medication and the relative effectiveness of DripDrop® as compared with other oral rehydration salts in preventing or reversing dehydration. As attested to by some key PEU staff, illustrated below, the results are clear, and striking:
Mrs Felicia Boakye-Agyeman, Matron-in-Charge of the Pediatric Emergency Unit at Komfo Anokye Teaching Hospital:
“Since DripDrop® Hydration Powder was received till now (a period of two months after the donation), the ward admitted 51 cases of diarrhea and vomiting. These children were given DripDrop® oral rehydration solution prepared at the unit. All 51 cases tolerated the drug very well, and over 90 percent of the cases had the diarrhea stopping completely within 24hrs. Unlike the other oral rehydration solutions, the DripDrop® solution has a very pleasant taste, and the children willingly consume adequate amounts with little no coaxing, thereby ensuring complete rehydration within a significantly shorter period.”
Dr. Maame Serwaa Asafo Agyei, a PEU pediatrician:
I observed that the DripDrop® oral solution causes the dehydration in the children to reduce and stop more promptly. I have also noted that because of the fruity taste of DripDrop® oral solution, the children are able to take in more, as compared with the other types of solutions, and this has helped to minimize the number of children eventually requiring intravenous fluids to correct their dehydration. The inclusion of zinc in the DripDrop® Hydration powder eliminates the additional zinc tablet that has to be added to the other oral rehydration solutions that have no zinc. This product is superb.
Now there has been a reduction in number of admissions of cases of diarrhea and vomiting, because when they such cases come to the PEU and the solution is prepared and given to them, their condition improves so quickly that they are discharged home with some of the drug. DripDrop® is a good drug that has come to support our interventions for diarrhea control. We thank Women’s Health to Wealth for the donation of the drug to the unit.
The usefulness of the DripDrop® Hydration Powder in addressing the rehydration of children with diarrhea and vomiting at the KATH PEU is worthy of note, as it not only reduces the workload of the already overworked staff, hospital costs and health bills for families but ultimately saves lives! Women’s Health to Wealth would like to acknowledge the support of our partner, AmeriCares, who made the supplies possible, and to WomenStrong International, which supports all the activities of WHW.
Nearly 50 per cent of all newborns develop a yellowing of skin and eyes known as jaundice. Newborn jaundice can occur when babies have a high level of a yellow pigment bilirubin produced during the normal breakdown of red blood cells. The high levels of bilirubin are due to the inability of the still- developing liver of the newborn to remove bilirubin.
In most cases the jaundice goes away on its own however the high levels of bilirubin can put a baby at risk for deafness, cerebral palsy or other forms of brain damage and ultimately death. The irreparable damage that can be caused by jaundice in the newborn therefore makes it important that all cases of jaundice are immediately detected and addressed by health providers. The levels of bilirubin can be detected through the skin or blood sample.
In Kumasi, jaundice in the newborn is responsible for the admission of up to one in every five babies at the two low-resource neonatal units and the Komfo Anokye Teaching Hospital (KATH) Mother-Baby-Unit Kumasi.
In KATH, the absence of the means of testing for levels of bilirubin in the unit, babies who show up with jaundice have to be admitted for tests. Mothers of babies admitted with jaundice have to pay between $6 and $8 USD to have the test performed in a laboratory to help doctors determine and confirm the treatment for the jaundiced baby. Laboratory tests typically have a turnaround time of 36 hours with the earliest being 24 hours for mothers who are able to afford it. Delay in early assessment of bilirubin levels due to mothers ability to pay for the test can result in situations where babies who could have been sent home are kept on the already overcrowded unit .
Women’s Health to Wealth (WHW) has been working with KATH to improve neonatal health outcomes. After a careful consideration of the costs of the existing situation in the current diagnosis of jaundice in the MBU decided to acquire some Transcutaneous Bilimeters (TCB)to facilitate the detection and treatment of neonatal jaundice.
With funding support from Women Strong International, a consortium of which WHW is a member, four pieces of TCB were purchased to facilitate the detection and assist in the timely management of neonatal jaundice.

Two pieces of the TCB were donated by WHW to the KATH MBU in June 2015. The equipment was received by the head of the unit, Dr. Gyikua Plange–Rhule in the company of her colleague and administrators. In her acceptance speech, she stressed on the speed of diagnosis and ultimately the efficiency that the equipment would bring to the treatment of sick babies and the unit. She also emphasized the budget relief that the equipment would bring to both mothers and the unit as the TCB can diagnose 500 patients at virtually the cost of 2 AA batteries. Her major concern was with the fragile nature of the black tip cover and the need for users to handle the equipment with care.
On her part, Nana Abenaa Akuamoa-Boateng the executive director of WHW thanked them for the opportunity to make a difference in the care of newborns with the provision of the diagnostic equipment. She however implored them to ensure that the usefulness of the tool is not hampered by the inability to replace the batteries that will cost the department less than $2 a month.
The two low resource MBU at the Kumasi South and Suntreso Hospitals in Kumasi have also been given one TCB each.
WHW wishes to appeal to well meaning individuals interested in donating TCBs to the remaining 35 district facility level hospitals in Ashanti to contact us.